Plantar fasciitis is one of the most common — and frustrating — causes of heel pain. That sharp, stabbing ache when you first step out of bed in the morning or after sitting too long can make everyday life a battle. The good news? You don’t have to put up with it. With the right mix of self-care, footwear, and practical strategies, you can ease the pain and stop it from coming back.
If you’ve been searching for how to get relief from plantar fasciitis, this guide brings together everything you need to know: causes, symptoms, immediate relief, longer-term fixes, and practical prevention.
“If foot pain is affecting your daily comfort, you might also find our Complete Guide to Foot Pain Relief helpful — it covers every cause and treatment in detail.”📌 At a Glance
All the key facts on Plantar Fasciitis in one place — no scrolling, no searching.
Jump straight down to the 20 quick Q&As at the bottom of this post.
What is Plantar Fasciitis?
The plantar fascia is a thick band of tissue running from your heel to your toes, supporting the arch of your foot. When it becomes overstretched or irritated, it causes tiny tears and inflammation — that’s plantar fasciitis.
Common Causes and Risk Factors
- Repeated stress from running, walking, or standing long hours
- Flat feet or very high arches that strain the fascia
- Wearing unsupportive shoes (flat, thin soles, or poor arch support)
- Sudden increase in activity (e.g. training too hard, too soon)
- Tight calf muscles or Achilles tendons
- Being overweight, which puts extra pressure on the fascia
If your arches have flattened or roll inward too much, that can add strain to the plantar fascia and heels.
It’s worth checking out: The Causes and Symptoms of Flat Feet
Heel pain isn’t always caused by plantar fasciitis — sometimes it’s a small bony growth under the heel called a heel spur, which can irritate the same tissues.
Learn more in our guide: Are Heel Spurs Painful?
Symptoms of Plantar Fasciitis
- Sharp heel pain, often worse first thing in the morning
- Pain after periods of rest that eases as you move
- Discomfort that increases with prolonged standing or activity
- Tenderness at the bottom of the heel
- Pain that sometimes radiates along the arch
Immediate Relief from Plantar Fasciitis
When the pain strikes, quick relief makes all the difference:
- Ice massage: Roll your foot over a frozen water bottle for 10–15 minutes.
- Rest and elevate: Limit impact activity and keep your foot raised to reduce swelling.
- Stretch your calves and arches: Gentle wall stretches or towel pulls can ease tension.
- Wide-fitting, cushioned shoes: Supportive footwear reduces strain instantly.
- Anti-inflammatory care: Over-the-counter gels or advice from a pharmacist may help.
Treatment and Long-Term Relief
Getting rid of plantar fasciitis for good usually takes a mix of strategies:
At-Home Care
- Regular calf and foot stretches to keep tissues supple
- Rolling your arch with a tennis or massage ball
- Supportive insoles or orthotics to distribute pressure evenly
- Night splints to keep the fascia gently stretched while you sleep
Professional Care
- Physiotherapy for strengthening and mobility exercises
- Custom orthotics after gait analysis
- Shockwave therapy or corticosteroid injections for persistent pain
- Surgery (rare and only for severe, unresponsive cases)
Why the Right Shoes Matter for Plantar Fasciitis
The wrong footwear is one of the fastest ways to aggravate plantar fasciitis — while the right shoes can be part of the solution.
Look for:
- Wide toe box to reduce pressure and allow natural toe spread
- Firm arch support to stop the fascia overstretching
- Cushioned midsoles for shock absorption
- Low to moderate heel-to-toe drop to ease pressure on the heel
- Removable insoles so you can insert orthotics if needed
Prevention Tips
- Break in new shoes gradually
- Replace worn shoes before the support “dies”
- Warm up and stretch before activity
- Avoid sudden jumps in training intensity
- Keep a healthy weight to reduce foot strain
- Alternate sitting and standing to avoid long periods of one or the other
When to See a Doctor or Podiatrist
- If pain persists beyond a few weeks despite self-care
- If it affects daily activities or mobility
- If swelling, redness, or numbness appear
- If you have diabetes or circulation issues and develop foot pain
👉 “To put plantar fasciitis into perspective, here’s a quick snapshot of how common it is in the UK and the impact it has on daily life.”
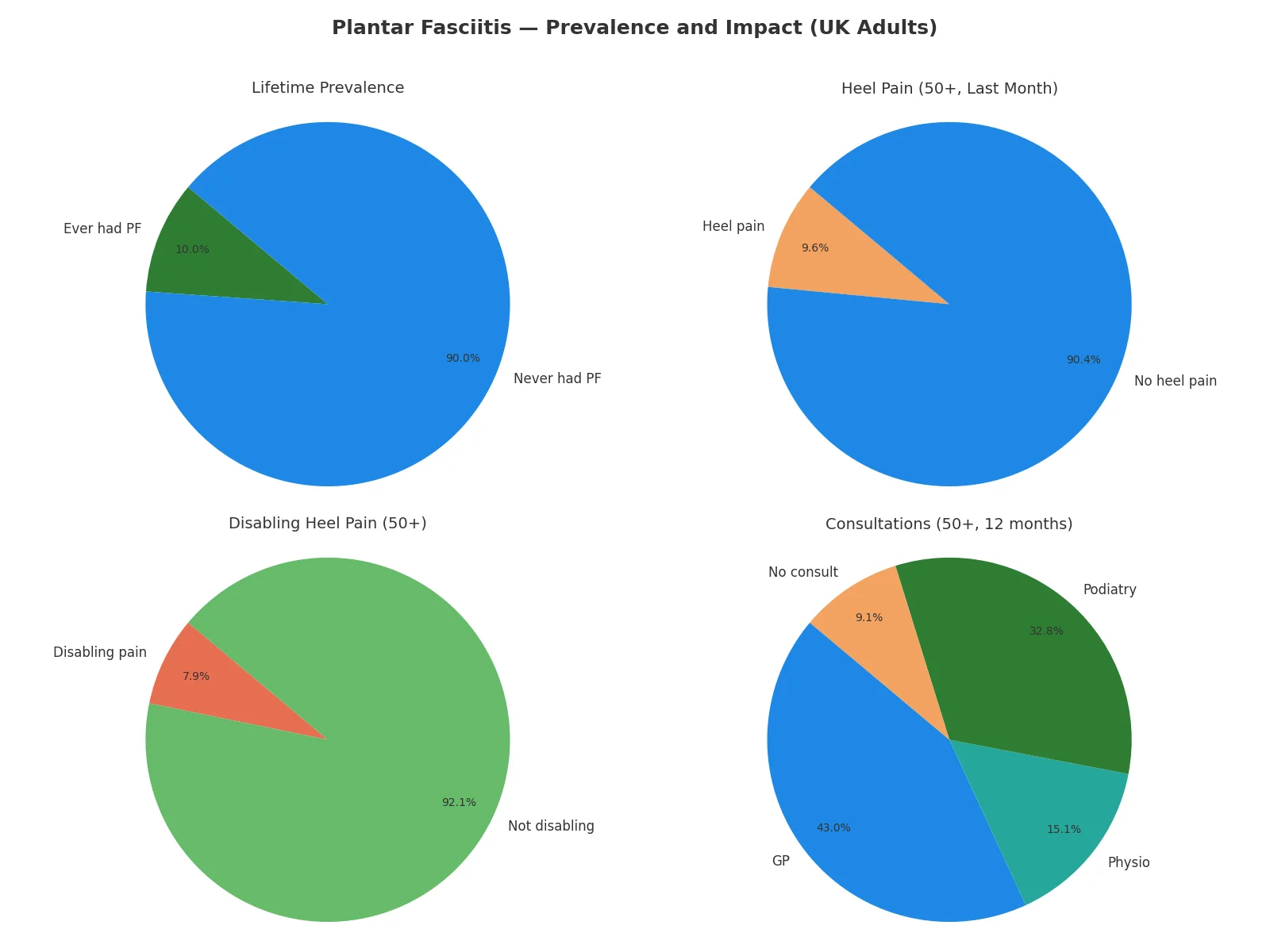
👉 “As the figures show, plantar fasciitis isn’t just a minor foot ache — it’s a widespread issue that affects mobility and quality of life, which makes finding effective relief all the more important.”
20 Common Questions on Plantar Fasciitis
Q: How do I know if my heel pain is plantar fasciitis?
A: The hallmark is sharp pain under the heel, worst in the morning or after rest, easing slightly as you walk.
Q: Can plantar fasciitis go away on its own?
A: Mild cases sometimes improve with rest, but most need a mix of stretching, footwear changes, and support to prevent recurrence.
Q: What’s the fastest way to relieve plantar fasciitis pain?
A: Ice, rest, and cushioned shoes usually provide the quickest relief. For long-term results, combine this with stretches and orthotics.
Q: Can I keep exercising with plantar fasciitis?
A: Low-impact activities like swimming or cycling are usually fine, but avoid running or high-impact sports until symptoms improve.
Q: Does losing weight help plantar fasciitis?
A: Yes. Reducing body weight decreases strain on the plantar fascia and speeds recovery.
Q: Are flip-flops bad for plantar fasciitis?
A: Yes, most are flat and unsupportive. Choose sandals with arch support and cushioning instead.
Q: Can tight calves cause plantar fasciitis?
A: Absolutely. Tight calves increase tension on the fascia, so stretching them daily helps.
Q: Are night splints really effective?
A: Many people find they reduce morning pain by keeping the fascia stretched overnight.
Q: What heel-to-toe drop is best for plantar fasciitis shoes?
A: A moderate drop (around 6–10mm) often works best, balancing heel relief with support.
Q: Does plantar fasciitis cause swelling?
A: Swelling isn’t typical. If your heel is swollen, it might be another condition such as bursitis.
Q: Can plantar fasciitis affect both feet?
A: Yes, although it often starts in one. The other foot can develop symptoms if strain continues.
Q: How long does it take to heal plantar fasciitis?
A: With proper care, many people improve in 6–12 weeks. Chronic cases may take several months.
Q: Are custom orthotics better than store-bought insoles?
A: Custom orthotics are tailored to your feet and can be more effective if off-the-shelf insoles don’t relieve symptoms.
Q: Can children get plantar fasciitis?
A: Rarely. It’s more common in adults, especially those over 40. Kids with heel pain may have Sever’s disease instead.
Q: Does plantar fasciitis cause toe pain?
A: The pain usually stays in the heel and arch, but tension can sometimes radiate toward the toes.
Q: Are rocker-sole shoes good for plantar fasciitis?
A: Yes, they help roll the foot forward smoothly, reducing heel impact.
Q: Can plantar fasciitis come back after it heals?
A: Unfortunately, yes. Without supportive shoes and stretches, recurrences are common.
Q: Is walking barefoot bad for plantar fasciitis?
A: On hard floors, yes — it increases strain. If you prefer barefoot, stick to soft, forgiving surfaces.
Q: Do compression socks help plantar fasciitis?
A: They can improve circulation and reduce swelling, but they don’t replace arch support.
Q: Should I see a podiatrist for plantar fasciitis?
A: Yes, if pain persists despite self-care. They can provide custom orthotics, therapies, and advice tailored to your feet.
✅ Summary
Plantar fasciitis is painful, but it’s also highly treatable. By making footwear changes, adding stretches, and knowing how to get relief from plantar fasciitis when it flares, you’ll be back on your feet with less pain and better comfort.